Researchers at Johns Hopkins Medicine are forging ahead with a groundbreaking new approach to Alzheimer’s disease treatment, bolstered by significant funding from the National Institutes of Health (NIH). Their latest study, published in the prestigious journal Proceedings of the National Academy of Sciences, zeroes in on a critical protein within the brain that, while perhaps best known for producing a gas with a distinctly unpleasant odor, appears to play a pivotal role in the very architecture of memory formation. This discovery opens a promising new avenue for understanding and potentially combating the devastating neurodegenerative effects of Alzheimer’s.
The Unlikely Hero: Cystathionine γ-lyase and Hydrogen Sulfide
The protein at the heart of this research is Cystathionine γ-lyase, or CSE. While commonly associated with the production of hydrogen sulfide (H₂S), the gas responsible for the characteristic smell of rotten eggs, its function extends far beyond olfactory unpleasantness. The Johns Hopkins team, led by Bindu Paul, M.S., Ph.D., an associate professor of pharmacology, psychiatry, and neuroscience, has demonstrated through experiments with genetically engineered mice that CSE and its gaseous byproduct are integral to how the brain consolidates memories.
"Our findings indicate that CSE is not merely a biochemical curiosity," stated Dr. Paul in a recent interview. "It appears to be a fundamental component of the neuronal machinery responsible for cognitive function. Disruptions in its activity, as we’ve observed, have profound implications for learning and memory."
The research aims to unravel the intricate mechanisms by which CSE operates and to determine if enhancing its activity could serve as a protective shield for brain cells, thereby slowing the progression of neurodegenerative conditions like Alzheimer’s.
A Protective Gas: The Dual Nature of Hydrogen Sulfide
Previous scientific endeavors had already hinted at the neuroprotective capabilities of hydrogen sulfide in laboratory settings. Studies had shown that H₂S could safeguard neurons in mouse models. However, the inherent toxicity of hydrogen sulfide in higher concentrations presented a significant hurdle. Direct administration to the brain was deemed unsafe, prompting scientists to explore alternative strategies. The focus shifted to understanding how to safely maintain the naturally occurring, extremely low levels of H₂S within neurons, levels that appear to be crucial for healthy brain function.
The current study provides compelling evidence for the importance of CSE. Mice genetically engineered to lack the CSE enzyme exhibited significant deficits in memory and learning. Furthermore, these mice displayed elevated levels of oxidative stress, increased DNA damage, and compromised integrity of the blood-brain barrier – all hallmarks commonly observed in individuals affected by Alzheimer’s disease.
"When we removed CSE from the equation, the consequences were stark," explained Dr. Paul, the study’s corresponding author. "The mice not only struggled with basic cognitive tasks but also showed cellular and structural changes in their brains that strikingly mirrored those seen in Alzheimer’s pathology. This strongly suggests a direct link between CSE deficiency and the neurodegenerative processes characteristic of the disease."
A Legacy of Research: Building on Decades of Discovery
This latest research is not an isolated breakthrough but rather a significant step forward, building upon years of foundational work by pioneering scientists at Johns Hopkins, most notably Solomon Snyder, M.D., D.Sc., D.Phil., a professor emeritus of neuroscience, pharmacology, and psychiatry. Dr. Snyder’s lab has been instrumental in illuminating the multifaceted roles of various gasotransmitters, including hydrogen sulfide, within the central nervous system.
As far back as 2014, Dr. Snyder’s team published findings in Nature detailing how CSE played a protective role in mice models of Huntington’s disease, another debilitating neurodegenerative disorder. These earlier studies utilized mice specifically engineered to be deficient in the CSE protein, a line of research that began in 2008 when CSE was first linked to critical functions in blood vessel health and blood pressure regulation.
The progression of this research continued. In 2021, the same group observed that CSE was not functioning optimally in mice genetically predisposed to Alzheimer’s disease. Crucially, they also found that administering very small, precisely controlled doses of hydrogen sulfide via injection helped to preserve cognitive function in these mice. This suggested a therapeutic potential for H₂S, albeit one that required careful modulation.
While the earlier studies often involved mice with additional genetic mutations associated with specific neurodegenerative diseases, the current work provides a more focused examination. By isolating the role of CSE itself, independent of other genetic factors, the researchers have been able to pinpoint its singular importance in cognitive processes.
"This most recent work indicates that CSE alone is a major player in cognitive function and could provide a new avenue for treatment pathways in Alzheimer’s disease," remarked Dr. Snyder, who retired from the Johns Hopkins Medicine faculty in 2023 but remains a key contributor to this ongoing research. "The ability to understand and potentially manipulate CSE offers a tangible target for therapeutic intervention."
Mapping Memory Decline: The Barnes Maze and CSE Deficiency
To rigorously investigate the impact of CSE on memory, the Johns Hopkins researchers employed a well-established behavioral paradigm: the Barnes maze. This test is designed to assess spatial learning and memory in rodents. The scientists compared mice engineered to lack the CSE protein with their normal littermates, utilizing the same genetically modified mouse strain that had been developed in 2008.
The Barnes maze involves mice learning to locate a hidden escape hole on a platform to avoid a mild, aversive bright light. The performance of both normal mice and CSE-deficient mice was monitored at different ages. At two months old, both groups performed similarly, successfully locating the escape route within a reasonable timeframe of three minutes. This indicated that in younger animals, the absence of CSE did not yet manifest as a significant cognitive deficit.
However, a stark divergence emerged by six months of age. The CSE-deficient mice began to struggle considerably, taking much longer to find the escape route, or in some cases, failing to do so altogether. In contrast, their normal counterparts continued to perform with efficiency, demonstrating robust spatial memory.
"The progressive decline in spatial memory observed in the CSE-deficient mice is a clear indicator of a neurodegenerative process that we can directly attribute to the loss of CSE," stated Suwarna Chakraborty, the study’s first author and a researcher in Dr. Paul’s lab. "This finding is particularly significant as it demonstrates a temporal aspect to the cognitive impairment, mirroring the gradual nature of Alzheimer’s disease progression."
Cellular Echoes of Alzheimer’s: Brain Changes in CSE-Deficient Mice
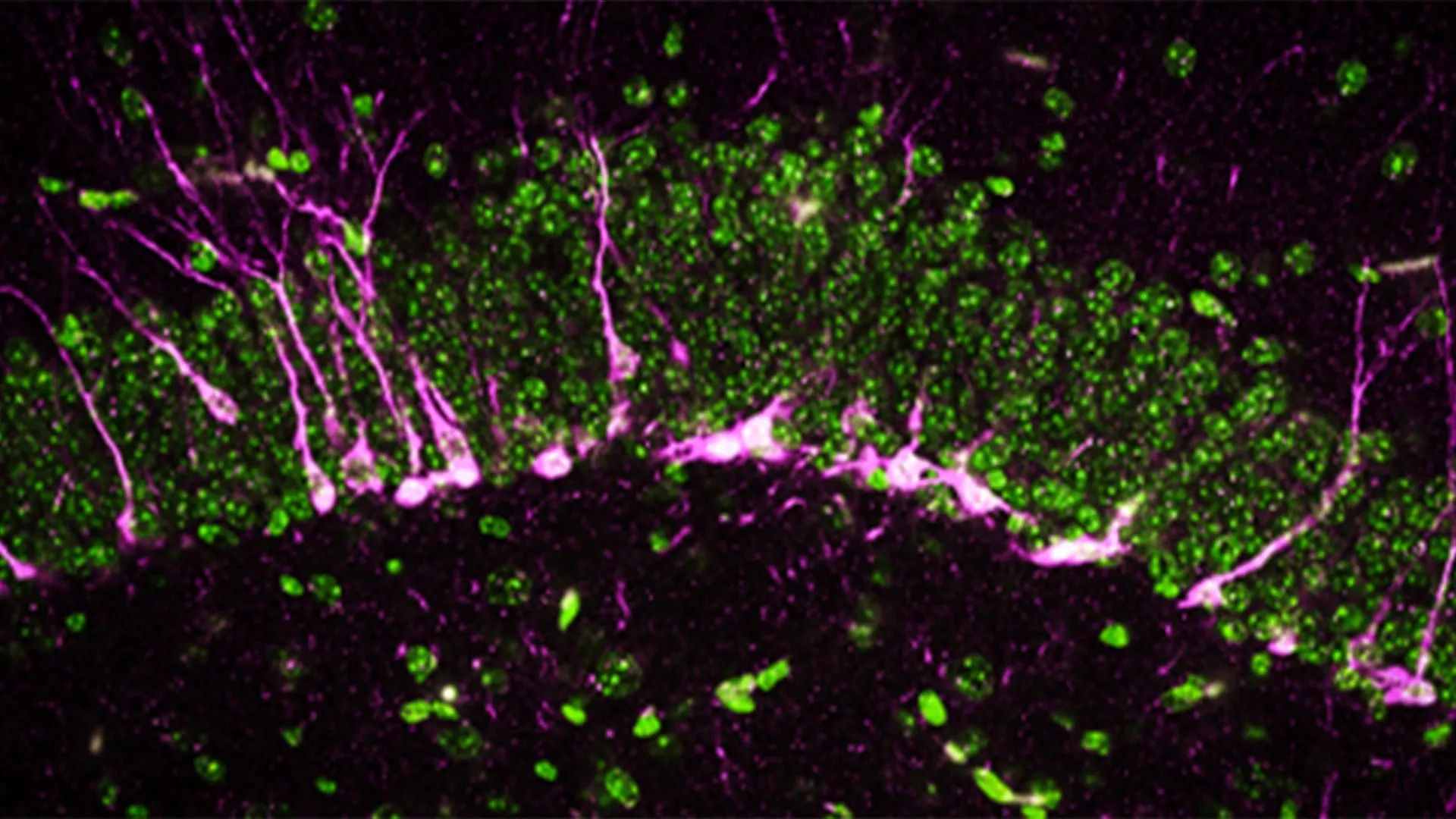
Beyond behavioral observations, the researchers delved into the cellular and structural consequences of CSE absence within the brain. They focused on the hippocampus, a brain region critically involved in the formation of new memories and a well-known site of pathology in Alzheimer’s disease. Neurogenesis, the process of generating new neurons, is essential for hippocampal function and is often impaired in neurodegenerative conditions.
Through a combination of sophisticated biochemical and analytical techniques, the team discovered that key proteins essential for neurogenesis were either reduced in quantity or entirely absent in the brains of mice lacking CSE. This cellular dysfunction directly impacted the brain’s ability to generate new nerve cells, a fundamental process for cognitive resilience.
Further examination using high-powered electron microscopes revealed striking structural abnormalities within the brains of these mice. The researchers observed significant disruptions in the integrity of blood vessels, indicating damage to the blood-brain barrier. This breakdown of the blood-brain barrier is another critical hallmark of Alzheimer’s disease, allowing potentially harmful substances from the bloodstream to enter the brain. Moreover, the study noted that newly formed neurons in these mice encountered difficulties in migrating to the hippocampus, hindering their integration into existing neural networks and their contribution to memory formation.
"The mice lacking CSE were compromised at multiple levels, from cellular processes to structural integrity," commented Sunil Jamuna Tripathi, a co-first author and researcher in Dr. Paul’s lab. "These multi-faceted deficits correlated strongly with the symptoms and pathological changes we observe in Alzheimer’s disease. It underscores the pervasive impact of CSE deficiency on brain health."
The Broad Implications: A New Frontier in Alzheimer’s Therapeutics
Alzheimer’s disease represents a monumental public health challenge. In the United States alone, it affects more than 6 million individuals, a number projected to rise significantly in the coming decades. The current landscape of Alzheimer’s treatments offers limited options, with no consistently proven therapies capable of halting or substantially slowing the disease’s relentless progression.
The findings from Johns Hopkins Medicine offer a beacon of hope. By identifying CSE and its role in hydrogen sulfide production as a potential therapeutic target, researchers are charting a new course for the development of novel treatments. The goal is to devise therapies that can protect vital brain functions and effectively slow the devastating march of neurodegeneration.
"Targeting the CSE pathway could provide a fundamentally different approach to Alzheimer’s treatment," explained Dr. Paul. "Instead of solely focusing on clearing pathological proteins, we can explore strategies to bolster the brain’s innate protective mechanisms. This could involve developing compounds that safely modulate CSE activity or enhance hydrogen sulfide signaling within neurons."
The implications extend beyond Alzheimer’s. Given that many neurodegenerative diseases share common pathological features, including oxidative stress and impaired neurogenesis, therapies developed targeting CSE could potentially benefit individuals suffering from a range of related conditions.
A Collaborative Endeavor: Funding and Research Partnerships
This pivotal research was made possible through substantial financial support from a consortium of leading scientific and governmental organizations. The National Institutes of Health provided crucial funding through several grants, including: 1R01AG071512, P50 DA044123, 1R21AG073684, O1AGs066707, U01 AG073323, AG077396, NS101967, NS133688, and P01CA236778. Additional support came from the Department of Defense (HT94252310443), the American Heart Association (including the AHA-Allen Initiative in Brain Health and Cognitive Impairment), the Solve ME/CFS Initiative, and the Catalyst Award from Johns Hopkins University. Further contributions were provided by the Valour Foundation, the Wick Foundation, a Department of Veterans Affairs Merit Award (I01BX005976), the Louis Stokes Cleveland Department of Medical Affairs Veterans Center, the Mary Alice Smith Funds for Neuropsychiatry Research, the Lincoln Neurotherapeutics Research Fund, the Gordon and Evie Safran Neuropsychiatry Fund, and the Leonard Krieger Fund of the Cleveland Foundation.
The extensive collaborative nature of this research is reflected in the diverse team of scientists involved. In addition to Dr. Paul, Dr. Snyder, Ms. Chakraborty, and Mr. Tripathi from Johns Hopkins, key contributors included Richa Tyagi and Benjamin Orsburn from Johns Hopkins. The study also benefited from the expertise of Edwin Vázquez-Rosa, Kalyani Chaubey, Hisashi Fujioka, Emiko Miller, and Andrew Pieper from Case Western University; Thibaut Vignane and Milos Filipovic from the Leibniz Institute for Analytical Sciences in Germany; Sudarshana Sharma from Hollings Cancer Center; Bobby Thomas from Darby Children’s Research Institute and the Medical University of South Carolina; and Zachary Weil and Randy Nelson from West Virginia University School of Medicine. This multidisciplinary approach, spanning institutions and specialized fields, underscores the complexity and significance of the research undertaken. The collective efforts of these researchers have laid a robust foundation for future investigations into CSE-based therapies for neurodegenerative diseases.